All About Breast Cancer in 2025
Physical Health

Breast cancer has the dubious distinction of being the most common type of cancer in women, and rates as the second most common cause of death from cancer among women worldwide. In this article, I will review the most up-to-date information about breast cancer, with an emphasis on what is new in 2025.
Incidence
Data from the American Cancer Society (ACS) and the World Health Organization (WHO) shed some light on the extent of the breast cancer problem:
- Breast cancer accounts for about 11.7% of all cancer diagnoses
- 13.1% (1 in 8) of women in the United States (US) will be diagnosed with breast cancer in their lifetime, but only 2.3% (1 in 43) will die from breast cancer
- In 2025, there will be an estimated 319,750 new cases of breast cancer diagnosed in the US, and an estimated 42,680 breast cancer-related deaths
- Breast cancer incidence rates for women in the US have been increasing since 2018, and reached an all-time high in 2021 of 144.6 per 100,000 people in the US. This is the most recent year that these data have been tabulated by the ACS
Breast cancer is far less common in men than in women. The ACS provides the following data for the incidence of breast cancer in men:
- In 2025, there will be an estimated 2,800 new cases of breast cancer diagnosed in men in the US, and 510 men will die from breast cancer
- Less than 1% of all breast cancers in the US occur in men
- The average lifetime risk of a man in the US getting breast cancer is about 1 in 755
- The average age of diagnosis of breast cancer among men in the US is 72 years
Prognosis/Outlook
The 5-year relative survival rate for newly diagnosed breast cancer of any stage is 91%. The “5-year relative survival rate” is a statistic that represents the percentage of people still alive 5 years after diagnosis compared to people of the same age and gender who do not have breast cancer.
The 5-year relative survival rate for breast cancer differs based on the stage of the cancer at the time of diagnosis:
- Localized breast cancer: This is cancer that is confined to a single breast and has not spread to lymph nodes or other organs. 99%
- Regional breast cancer: This is where the cancer has spread to nearby lymph nodes but not to distant parts of the body. 87%
- Distant breast cancer: The cancer has spread to body tissues outside the immediate area of the breasts and lymph nodes, such as the liver, bones, lungs, or brain. 32%
The death rate from breast cancer remained stable in the US at between 30 and 34 deaths per 100,000 population until 1990, and it has been steadily declining since, reaching a low of 18.7 deaths per 100,000 population in 2021 (the last year the ACS tabulated these data).
Breast Cancer Risk Factors
Risk factors for breast cancer in women include:
- Female gender
- Increasing age
- Inheriting certain gene mutations (such as BRCA1 and BRCA2 gene mutations)
- A family history of breast cancer
- Being taller
- Having dense breasts
- Starting periods at a younger age
- Later menopause
- Radiation exposure to the chest
- Alcohol use
- Being overweight or obese
- Being physically inactive
- Not having children
- Not breastfeeding
- Hormone replacement therapy*
(*Whether and the extent to which HRT is a risk factor for breast cancer is dependent upon a woman’s other baseline risk factors and the specifics related to her HRT which is why it is crucial to discuss your individual case and the risks and benefits of HRT with your physician.)
Among men, most who develop breast cancer have no known risk factors. However, additional risk factors that apply to men include:
- Klinefelter syndrome (a chromosomal disorder with an abnormal number of sex chromosomes)
- Liver disease
- Estrogen hormonal treatments (such as in transgender men)
- Certain testicular conditions
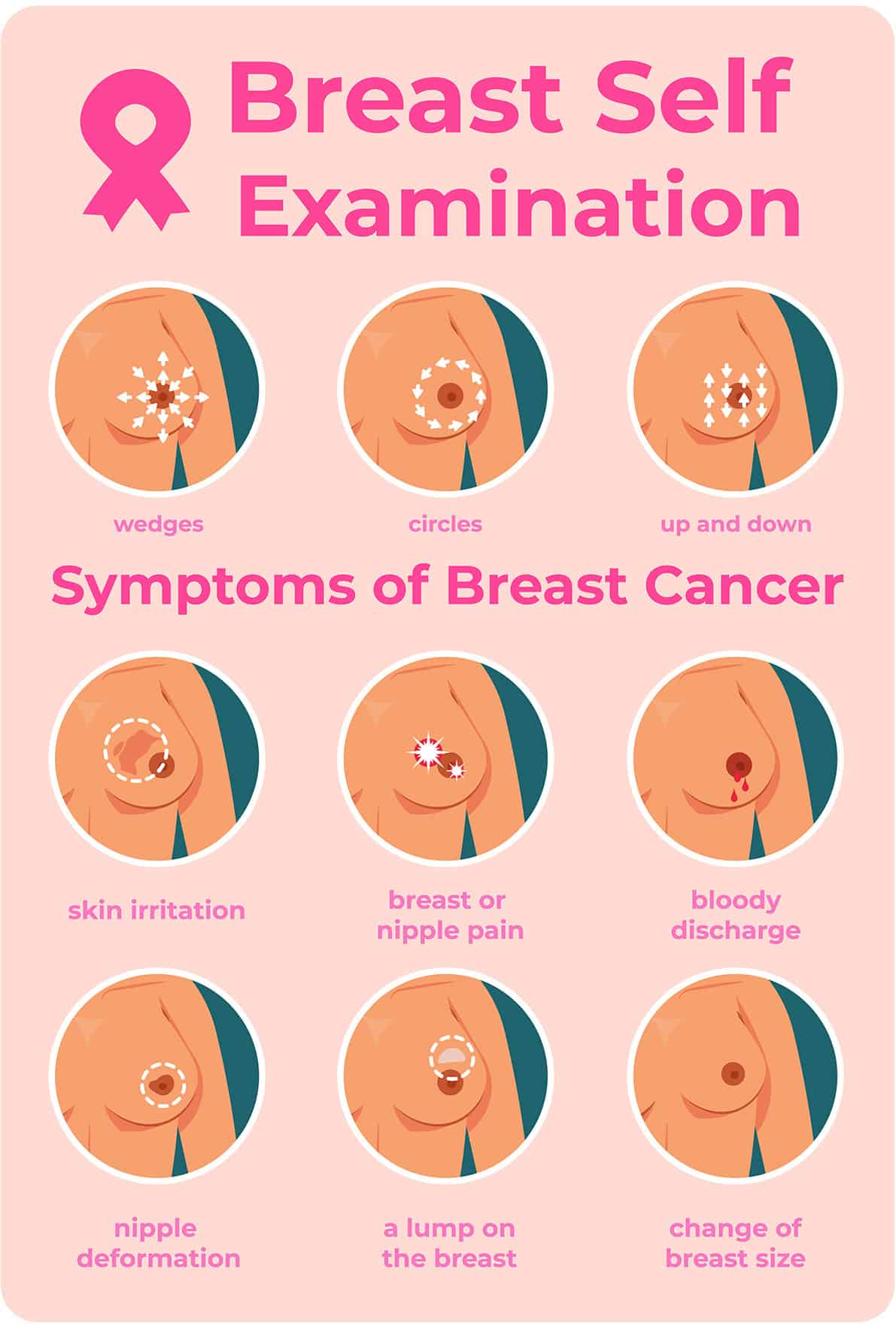
Breast Cancer Symptoms
The symptoms of breast cancer include:
- A new breast lump
- New thickening or swelling in a breast
- Breast skin that looks dimpled, like an orange peel (“peau d’orange skin”)
- A change in size, shape, or appearance of a breast
- A nipple that turns inward or flattens
- Breast or nipple pain
- Non-milk nipple discharge, especially if bloody
- Breast skin or nipple that is thickened, red, dry, warm, or flaking
- Swollen lymph glands in the armpit or along the collarbone
Types of Breast Cancer
I discussed breast cancer stages based on the degree of spread in the prognosis/outlook section above. However, there are different types of breast cancer, and they are generally classified as follows:
- Non-invasive breast cancer: These can be either ductal carcinoma in situ (DCIS) or lobular carcinoma in situ (LCIS), depending on the type of breast cells that they arise from. These are early-stage, localized cancers that have not yet spread beyond the tissues from which they originated
- Invasive breast cancer: These are tumors that have spread to other breast tissues or nearby lymph nodes (i.e., regional spread). They may be invasive ductal carcinoma (IDC) or invasive lobular carcinoma (ILC)
- Metastatic breast cancer: These are advanced cases of breast cancer that have spread to other body organs (i.e., distal spread)
There are other rare types of breast cancer, including:
- Inflammatory breast cancer (IBC): These account for 1-5% of cases of breast cancer. This is an aggressive form of cancer. It causes the breast to become red and swollen (inflamed).
- Paget’s disease of the breast: This cancer starts in the breast ducts and spreads to the nipple and areola. These account for 1-3% of cases of breast cancer.
- Angiosarcoma: These cancers arise in the blood vessels and lymph ducts of the breast or overlying skin. They account for less than 1% of all cases of breast cancer. They often arise after radiation exposure to the breast.
- Triple-negative breast cancer: These are not rare, comprising about 10-15% of new breast cancer diagnoses. These tumors are without receptors for the female sex hormones estrogen and progesterone, and the human epidermal growth factor-receptor 2 (HER-2) protein. This is an invasive breast cancer that tends to grow and spread rapidly.
Breast cancer is often further classified according to receptors that are found on the cancer cells. This is because the presence or absence of these receptors affects prognosis and choice of treatments. The primary receptors of concern are estrogen receptors (ER) and progesterone receptors (PR), as well as HER2 receptors.
Breast Cancer Diagnosis
Early diagnosis is a major focus of public health, given the excellent prognosis for early-stage breast cancer that is still in situ and localized. Screening guidelines differ somewhat between authoritative institutions. The US Preventive Services Task Force, whose guidelines were updated in April 2024, recommends that “all women get screened for breast cancer every other year, starting at age 40 and continuing through age 74.”
The 2023 ACS breast cancer screening guidelines are more detailed. These recommend the following for women of average risk:
- Women aged 40 to 44 have the option to start screening with an annual mammogram every year
- Women aged 45 to 54 should get annual mammograms
- Women 55 and older may continue with annual mammograms or switch to a mammogram every other year
- Breast cancer screening should continue as long as the individual is in good health and is expected to live at least 10 more years
- Clinical breast exams for women of average risk are not recommended for breast cancer screening
The ACS website defines high-risk individuals and describes the recommended screening for these women.
If the screening identifies a breast mass of concern, then diagnostic testing is used to diagnose or rule out breast cancer. This may include:
- A medical history: Your physician will take an overall health history, asking about your overall health, your risk factors for breast cancer, your personal and family history of cancer, your medications, any symptoms of breast cancer you may have had, and so on.
- A physical exam: Your physician will examine your breasts and your overall body, paying close attention to the signs of breast cancer or spread.
- Diagnostic mammogram: This is a more detailed version of the screening mammogram, with extra compression and views of the area in question.
- Breast magnetic resonance imaging (MRI) scan: This is a detailed scan of the breasts that uses no radiation. A gadolinium-based contrast agent (GBCA) is given through an intravenous infusion to enhance the clarity of the scan.
- Biopsy: Different types of biopsy options are available to get tissue for definitive diagnosis. These may be performed via fine-needle aspiration (FNA), core biopsy (CB), or vacuum-assisted core biopsy (VACB), which use needles to obtain a sample of the lesion of concern. Alternatively, an incisional biopsy may be obtained by cutting through the overlying skin, or an excisional biopsy to remove the entire lesion.
- Lab tests: Biopsy results will be tested in the lab to determine the tumor type and its receptor status. Blood samples will be taken to check the individual’s overall health and to conduct genetic testing to look for breast cancer genes. This will stratify the person’s risk and allow for genetic counseling regarding their relatives.
Breast Cancer Treatment

Breast cancer treatment is heavily personalized, based on the type and stage of the tumor, the receptors present on the cancer cells, the patient’s overall health and ability to tolerate treatment, and patient preferences. The following may be treatment options:
- Lumpectomy: Surgical removal of all the cancer tissue while sparing the rest of the breast.
- Mastectomy: Removal of all breast tissue. One or both breasts may be removed.
- Lymph node biopsies: This may involve just sampling some lymph nodes from under the arm (sentinel lymph node biopsy—SLNB), or by taking many of them (axillary lymph node dissection—ALND).
- Cryoablation: Destroying cancer cells by freezing them without surgery.
- Radiation therapy: This may be used after surgery to destroy any remaining cancer cells, or to treat cancer that has spread to other parts of the body (metastases).
- Chemotherapy: This involves using drugs that are toxic to breast cancer cells. It may be used before surgery (neo-adjuvant chemotherapy) or after surgery (adjuvant chemotherapy). Chemotherapy may also be used to treat metastases.
- Targeted drug therapy: These are “precision” drugs that target specific biochemical features that are unique to cancer cells.
- Immunotherapy: These are drugs that help the patient’s own immune system become more effective at targeting cancer cells.
- Hormone therapy: These are drugs that block hormone receptors on tumors that use hormones to grow.
In most cases, an individual’s treatment plan will include a combination of these treatment options tailored to their specific situation. The treatment may be adjusted depending on how their cancer responds to the initial treatment, or if there is any post-treatment recurrence.
What’s New in 2025?
The American Society of Clinical Oncology (ASCO) provided its annual update on breast cancer at its June 2025 conference. The highlights include:
- New drug therapies: Several new drugs have been approved by the Food and Drug Administration (FDA) for treating breast cancer. For example, the targeted therapy Datroway (datopotamab deruxtecan) was approved for treating advanced HR+/HER2- breast cancer, having shown significant reductions in disease progression and mortality compared to standard chemotherapy.
- New combination therapies have been tried and confirmed, especially for triple-negative breast cancer, which has fewer treatment options.
- Clinical trials: New clinical trial results have been published, with significant findings regarding the safety of hormone therapy for women with breast cancer, and new genetic testing recommendations.
- Screening and diagnosis: Studies are underway evaluating the use of 3-D mammography in place of the currently used 2-D mammography for early diagnosis, and evaluating the use of contrast dye to improve screening effectiveness in women with dense breasts.
In 2025 the FDA has also removed the black box warning for HRT in women. The removal of these black box warnings regarding HRT for women will be initiated as they relate to the risk of cardiovascular disease, breast cancer, stroke and probable dementia. The boxed warning regarding the systemic use of unopposed estrogen in women with a uterus will remain. It is important to remember that this risk is mitigated by adding progesterone to one’s HRT regimen.